Navigating life with ulcerative colitis (UC) can be challenging, especially when it comes to managing your diet. As a chronic inflammatory bowel disease affecting the colon and rectum, UC often leads to unpredictable flare-ups and periods of remission. A well-thought-out ulcerative colitis diet plan is crucial for minimizing symptoms, promoting gut health, and achieving long-term wellness. Diet plays a key role in influencing the disease course, maintaining remission, and managing symptoms, though individual responses vary. Whether you’re searching for “what to eat during a UC flare” or “best foods for UC remission,” this comprehensive guide provides evidence-based recommendations for you.
UNDERSTANDING ULCERATIVE COLITIS AND THE ROLE OF DIET
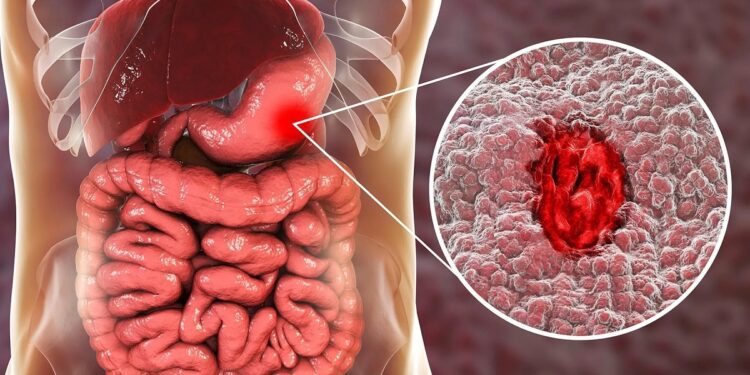
Ulcerative colitis is an inflammatory bowel disease (IBD) that causes long-lasting inflammation and ulcers in the digestive tract, primarily the colon. Symptoms include abdominal pain, diarrhea (often bloody), urgency, fatigue, and weight loss. While the exact cause is unknown, it involves immune system dysregulation, genetics, and environmental factors.
Diet does not cause UC, but it significantly impacts symptom management and quality of life. As noted by the NIDDK, no specific foods are proven to cause or worsen UC, but a healthy, balanced diet can help reduce risks and support overall health. During flares, the focus shifts to gentle, easy-to-digest foods to soothe the gut, while remission allows for a broader, anti-inflammatory diet to prevent relapses.
Anemia: Types, Causes, Symptoms & Effective Treatment Options
Personalization is key—track your intake with a food journal to identify triggers. Consult a registered dietitian specializing in IBD for tailored advice, as restrictive diets can lead to nutrient deficiencies. Emerging research highlights diets like the Mediterranean or low-FODMAP for potential benefits, but evidence is mixed.
ULCERATIVE COLITIS DIET DURING A FLARE: SOOTHING YOUR GUT
An Ulcerative colitis flare-up can be debilitating, with increased inflammation leading to severe symptoms. The goal of a diet during Ulcerative colitis flare is to reduce irritation, prevent dehydration, and ensure nutrient absorption without exacerbating diarrhea or pain. Opt for a low-residue or low-fiber diet to minimize bowel movements and give your colon a rest.
FOODS TO EAT DURING ULCERATIVE COLITIS FLARE
Prioritize soft, nutrient-dense foods that are easy on the digestive system. It is adviced to focus on low-fiber fruits, lean proteins, refined grains, and cooked vegetables without seeds or skins. These provide essential vitamins, minerals, and calories while being gentle.
- Low-Fiber Fruits: Bananas, applesauce, peeled or cooked apples/pears, honeydew melon, papaya, blended fruits like smoothies. These offer potassium and hydration without roughage.
- Cooked Vegetables: Asparagus tips, fork-tender carrots, green beans, squashes, potatoes (peeled and mashed), cucumbers (peeled). Cooking breaks down fibers for easier digestion.
- Lean Proteins: Chicken, turkey, fish (like salmon for omega-3s), eggs, firm tofu, nut butters (smooth, not chunky). Protein needs increase during inflammation, states University Hospitals.
- Refined Grains: Oatmeal, white rice, sourdough bread, white pasta, crackers. These are low in insoluble fiber and provide energy.
- Dairy Alternatives (if tolerated): Lactose-free yogurt, almond or oat milk fortified with calcium and vitamin D.
- Other Soothing Options: Hummus, guacamole, olive oil-based pesto, bone broth, oral rehydration solutions for hydration. Incorporate liquid meals like soups and smoothies during flares for their soothing properties
Aim for small, frequent meals—five to six per day—to avoid overwhelming the gut.
Bone Fractures: Types, Causes, Symptoms & Treatment Options
FOODS TO AVOID DURING A UC FLARE
Certain foods can irritate the inflamed colon, worsening symptoms. Some food to avoid are:
- High-Fiber Foods: Raw vegetables (e.g., broccoli, cauliflower, kale), whole grains, bran cereals, popcorn, nuts, seeds.
- Dairy Products: Milk, cheese, ice cream (if lactose intolerant) as these may increase diarrhea and gas.
- Fatty and Greasy Foods: Fried items, butter, red meat, processed meats like bacon or sausages.
- Sugary and Processed Foods: Candy, pastries, ultra-processed snacks, sugary drinks—these can cause bloating and diarrhea.
- Spicy Foods: Chili, sriracha, hot sauces.
- Beverages: Alcohol, caffeine (coffee, tea), carbonated drinks, fruit juices with pulp.
- Other Triggers: Legumes (beans, lentils if not tolerated), cruciferous veggies, fruits with skins/seeds.
TIPS FOR MANAGING DIET DURING FLARES
- Stay hydrated: Drink water, broths, or electrolyte solutions to combat dehydration from diarrhea.
- Prepare in advance: Batch-cook and freeze meals for convenience.
- Supplement wisely: Consider omega-3s, probiotics, calcium, and vitamin D if deficient—consult your doctor.
- Eat mindfully: Chew thoroughly, eat slowly, and avoid eating late at night.
A 2020 study by Healthline suggests that adjusting to a low-fat, high-fiber diet post-flare may aid remission, but start low-fiber during active symptoms.
ULCERATIVE COLITIS DIET DURING REMISSION: BUILDING RESILIENCE
Remission is a time to nourish your body, reduce inflammation, and prevent future flares. A UC remission diet should be expansive, focusing on anti-inflammatory foods while reintroducing variety. As much as possible, keep your diet as broad as you can, especially with plant-based foods, to support gut health.
Foods to Eat During Remission
Emphasize nutrient-rich, anti-inflammatory options such as Mediterranean diet for its sustainability and remission-maintaining benefits:
- Fruits and Vegetables: Berries (raspberries, blueberries), leafy greens (cooked or blended), avocados, mangoes, peeled fruits. Gradually add high-fiber varieties.
- Whole Grains: Oats, brown rice, quinoa, whole-wheat bread (if tolerated).
- Lean Proteins: Fish (salmon, tuna for omega-3s), chicken, turkey, eggs, tofu, edamame, legumes.
- Healthy Fats: Olive oil, walnuts, chia seeds, flaxseeds, avocado.
- Dairy or Alternatives: Yogurt (probiotic-rich), cheese in moderation, plant-based milks.
- Other: Herbs, spices (mild), fermented foods like kimchi or miso for gut bacteria.
Cushing’s Syndrome: Causes, Symptoms, Diagnosis & Treatment Options
Foods to Avoid During Remission
Even in remission, limit potential triggers to maintain stability. These include:
- Processed and Red Meats: Bacon, deli meats, beef—linked to higher inflammation risk.
- High-Fat Foods: Fried items, coconut oil, palm oil.
- Sugary Foods: Pastries, sodas, artificial sweeteners (e.g., sucralose).
- Other: Raw cruciferous veggies if they cause gas, caffeine, alcohol in excess.
Tips for Diet in Remission
- Reintroduce foods slowly: Start with small portions to test tolerance.
- Focus on variety: Aim for 30g of fiber daily.
- Meal prep: Plan balanced meals with protein, carbs, and fats.
- Consider specialized diets: Low-FODMAP for persistent symptoms or paleo for some.
SAMPLE MEAL PLANS FOR ULCERATIVE COLITIS
Flare Meal Plan (Low-Residue Focus)
- Breakfast: Oatmeal with banana and almond butter.
- Snack: Applesauce and lactose-free yogurt.
- Lunch: Grilled chicken with mashed potatoes and cooked carrots.
- Snack: Smoothie with blended fruit and tofu.
- Dinner: Baked salmon with white rice and zucchini.
- Dessert: Gelatin or pudding.
Remission Meal Plan (Mediterranean-Inspired)
- Breakfast: Spinach and tomato scramble with whole-grain toast.
- Snack: Greek yogurt with berries.
- Lunch: Chicken power bowl with quinoa, veggies, and olive oil.
- Snack: Oatmeal banana bars.
- Dinner: Grilled fish with sweet potatoes and salad.
- Dessert: Fresh fruit or dark chocolate.
Long-Term Strategies for UC Diet Management
- Nutritional Supplements: Address deficiencies in iron, B12, or folate with doctor guidance.
- Lifestyle Integration: Combine diet with stress management (yoga) and exercise.
- Monitoring: Regular check-ins with a dietitian; avoid self-restriction to prevent malnutrition.
- Cultural Adaptations: Modify favorite recipes, e.g., use lean proteins in traditional dishes.
Ulcerative Colitis: Causes, Symptoms, Treatment & Long-Term Care
Empowering Your Ulcerative Colitis Journey Through Diet
A strategic ulcerative colitis diet plan can transform your experience with ulcerative colitis, easing flares and sustaining remission. By focusing on gentle foods during active periods and anti-inflammatory choices in calm times, you can reduce symptoms and enhance well-being. Remember, what works for one may not for another—track, consult experts, and be patient.
Hepatitis A, B & C: Causes, Symptoms, Transmission & Treatment